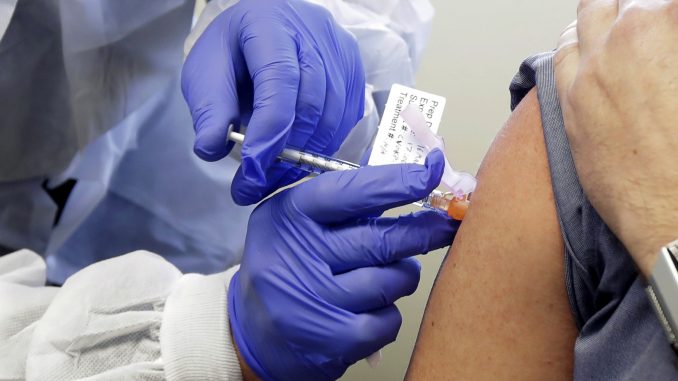
The first experimental COVID-19 vaccine in the U.S. is on track to begin a huge study next month to prove if it really can fend off the coronavirus, while hard-hit Brazil is testing a different shot from China.
Where to do crucial, late-stage testing and how many volunteers are needed to roll up their sleeves are big worries for health officials as the virus spread starts tapering off in parts of the world.
Moderna Inc. said Thursday the vaccine it is developing with the National Institutes of Health will be tested in 30,000 people in the U.S. Some will get the real shot and some a dummy shot, as scientists carefully compare which group winds up with the most infections.
With far fewer COVID-19 cases in China, Sinovac Biotech turned to Brazil, the epicenter of Latin America’s outbreak, for at least part of its final testing. The government of São Paulo announced Thursday that Sinovac will ship enough of its experimental vaccine to test in 9,000 Brazilians starting next month.
If it works, “with this vaccine we will be able to immunize millions of Brazilians,” said São Paulo´s Gov. Joao Doria.
Worldwide, about a dozen COVID-19 potential vaccines are in early stages of testing. The NIH expects to help several additional shots move into those final, large-scale studies this summer, including one made by Oxford University that’s also being tested in a few thousand volunteers in Brazil.
There’s no guarantee any of the experimental shots will pan out.
But if all goes well, “there will be potential to get answers” on which vaccines work by the end of the year, Dr. John Mascola, who directs NIH’s vaccine research center, told a meeting of the National Academy of Medicine on Wednesday.
Vaccines train the body to recognize a virus and fight back, and specialists say it’s vital to test shots made in different ways — to increase the odds that at least one kind will work.
Sinovac’s vaccine is made by growing the coronavirus in a lab and then killing it. So-called “whole inactivated” vaccines are tried-and-true, used for decades to make shots against polio, flu and other diseases — giving the body a sneak peek at the germ itself — but growing the virus is difficult and requires lab precautions.
The vaccine made by the NIH and Moderna contains no actual virus. Those shots contain the genetic code for the aptly named “spike” protein that coats the surface of the coronavirus. The body’s cells use that code to make some harmless spike protein that the immune system reacts to, ready if it later encounters the real thing. The so-called mRNA vaccine is easier to make, but it’s a new and unproven technology.
Neither company has yet published results of how their shots fared in smaller, earlier-stage studies, designed to check for serious side effects and how well people’s immune systems respond to different doses.
Even before proof that any potential vaccine will work, companies and governments are beginning to stockpile millions of doses so they can be ready to start vaccinating as soon as answers arrive.
In the U.S., a program called “Operation Warp Speed” aims to have 300 million doses on hand by January. Under Brazil’s agreement with Sinovac, the Instituto Butantan will learn to produce the Chinese shot.